Orthodontic treatment in young children with innovative soothers


Summary
Dental malpositioning, such as anterior open bites, posterior crossbites, and functional disruptions, such as persistent infantile swallowing patterns, are common in young children. These conditions are often caused or exacerbated by habits like thumb sucking or the use of baby bottles. This case series aims to demonstrate the effects of a new type of soother on the development of open bites, crossbites, and tongue dysfunction. The early treatment of these conditions is described using three selected cases, involving children between the ages of two and five.
During observation periods of three months, nine months, and two years, anterior open bites were closed, and posterior crossbites were alleviated. Additionally, the transition from a persistent infantile swallowing pattern to an adult swallowing pattern was observed. Initial results are promising; the method is straightforward and could potentially reduce costs. However, due to the small number of cases, reproducibility of these results cannot yet be confirmed, requiring further verification through a follow-up study involving a larger population.
Suckling behavior has been observed even in the womb, with the first signs appearing between the 15th and 18th weeks of pregnancy.1 By the 34th week, the ability to suckle is fully developed.2 In newborns, the suckling reflex can be stimulated by touching the lips or tongue, which encourages the infant to continue feeding.3 Mechanical-sensory stimulation, such as using a soother, triggers this reflex through the trigeminal nerve.4 Through repeated use, these movement patterns become established. Suckling serves purposes beyond just nutrition—it also helps to calm the infant, aid sleep, and relieve tiredness or boredom.5 Babies may use bottles, thumbs, fingers, nappies, bedding, and other objects for this purpose. In Switzerland, 80% of children between the ages of one and two use a soother, while almost 20% suck on other objects. More than half of children continue this habit until ages three or four, 35% at age five, and 5% at age seven.5
It is well known and well documented that using soothers can lead to dental and orthodontic misalignment.6,7,8,9 These issues can result in lengthy and expensive orthodontic treatments. Improper jaw development can also impact language development due to altered myofunctional processes. At the Sprachheilpädagogischen Förderzentrum, a speech therapy center in Rostock, only 7% of patients with abnormal speech development showed normal orthodontic growth.10 During breastfeeding, infants must stabilize the mother’s nipple using a forward movement of the lower jaw to efficiently take up milk. This movement strengthens the muscles in the mouth, tongue, and jaw, leading to better language development than in children who are bottle-fed.11 By contrast, frequent use of a bottle leads to persistent infantile swallowing patterns (tongue thrusting), as the tongue must regulate the amount of liquid released. The round shape and texture of the synthetic teat push the tongue downwards.
Negative pressure is needed to draw liquid into the mouth, and this action also pulls the cheeks inward. However, when the tongue is positioned at the bottom of the mouth rather than against the gums, it does not support the teeth. The inward pressure affects the dental arch and prevents or reverses transversal growth, potentially leading to the formation of a side crossbite. Furthermore, the round shape of the teat can promote the development of an open bite. Tongue thrusting keeps the open bite from closing by displacing the anterior teeth, which can contribute to lisping.
Side crossbites, backward displacement of the lower jaw, and tongue displacement during swallowing and speech can also occur.8 Since children typically suckle during their first years of life, the question arises: what is the best object for them to suck on? The ideal object should satisfy the infant’s need to suck without compromising or disrupting jaw growth or dental health.5 Ideally, suckling should cease once all milk teeth have erupted, around the age of two and a half. The side effects of soothers depend on the duration of use and the morphology of the soother. Some modified soothers may reduce the likelihood of developing an open bite (e.g., Dentistar, by Novatex, Germany). The new Curaprox soother (Curaden, Switzerland, distributed by Oral Science in Canada) claims to promote a different pressure distribution on the upper jaw compared to older models. Its flat design mimics the natural flat shape of the oral cavity during suckling, which may help prevent open bites. The soft central semicircle, which is squeezed by the baby’s tongue, generates transversal pressure that could prevent the narrowing of the upper jaw and crossbites. The lip plate sits away from the lower jaw, providing space for lip muscles to function freely without pushing the lower jaw backward. In the following selected cases, the effectiveness of pressure distribution is explored not only as a preventative measure but also as a therapeutic intervention.
Material and method
A survey was conducted at the beginning of this study to determine whether a baby bottle, soother, or other object was used for suckling. The size two test soother features a triangular shape that tapers into a shaft that is 20 mm wide at its narrowest point. The mouthpiece measures 25 mm at its widest point. From the plate attachment to the most anterior point, the length is 23 mm, with a narrow section of 21 mm in the middle. Additionally, there is a semicircular elevation extending in both lingual and palatal directions, with a diameter of 10 mm. The side wings are 4 mm thick, and both semicircles total 10 mm in height. The side wings have recesses at their edges that can align with the teeth in children with narrow upper jaws. To ensure effectiveness, no other objects were used for suckling.
Baby bottles were replaced by cups or bottles with an opening of at least 15 mm, such as a mineral water bottle. The test soother was used at least every night or to fall asleep.
Fig. 1

Fig. 2
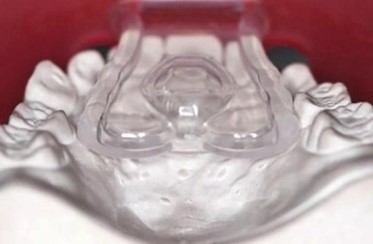
Fig. 3

Case reports
Case 1
A patient at the Schulzahn Clinic in Basel, aged four years and two months, presented with an open bite. She continued to use a baby bottle (at night and for comfort) and had significant plaque buildup. She had recently stopped using a soother. The patient exhibited a 7 mm open bite and mouth breathing (the molars had occlusal contact, and tooth 75 was missing), along with a persistent infantile swallowing pattern. Brushing frequency was increased, and the baby bottle was replaced with a size two Curaprox soother (Curaden, Switzerland, distributed by Oral Science in Canada). No further functional therapy was provided. During follow-up, the open bite reduced to 5 mm after six weeks, to 2 mm after five months, and finally to a normal overbite after nine months, along with improved oral hygiene. The swallowing pattern also changed from visceral to adult swallowing action. The new soother was well accepted by both the parents and the child, and transitioning from the bottle to the soother was smooth. The child had no difficulty giving up the soother after nine months of treatment.
Fig. 4
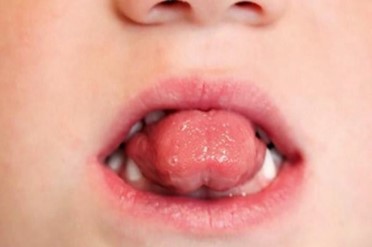
Fig. 5
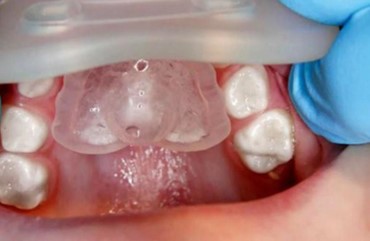
Fig. 6
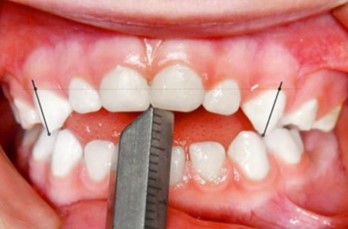
Fig. 7
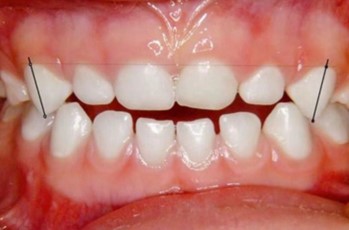
Fig. 8
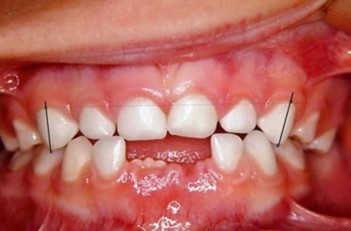
Fig. 9
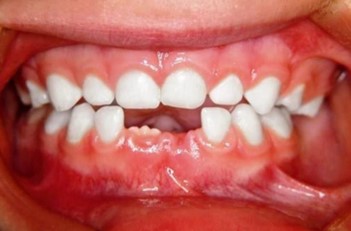
Case 2
A girl, aged four years and six months, was presented at the Schulklinik in Basel for the second time. During her first visit around the age of one, the recommendation to wean her off the dummy was not implemented. She continued to use the dummy to sleep, and a year later, her father brought her back to the clinic. He had noticed changes in her dental alignment. Morphologically and functionally, she presented with an open bite, edge-to-edge bite on teeth 53 and 83, and a crossbite on teeth 63 and 73. No persistent infantile swallowing pattern was present. The baby bottle was no longer used. The patient’s dummy was swapped for a size one Curaprox soother, which was used to fall asleep. After one month, it was replaced with a size two Curaprox soother. Within three months of treatment, the open bite was significantly reduced, and the edge-to-edge/crossbite of the milk canines was corrected. After two years of therapy, the patient displayed a normal overbite of the primary anterior teeth, and the edge-to-edge/crossbite of the canines was fully corrected. The soother was well accepted during the entire treatment period and weaning her off the soother posed no issues.
Fig. 10
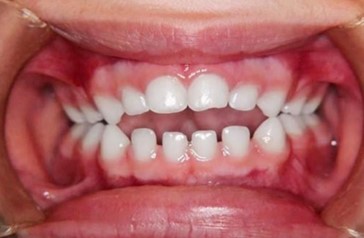
Fig. 11
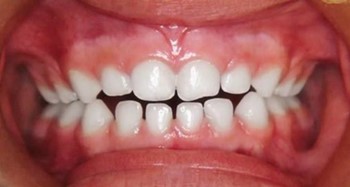
Fig. 12
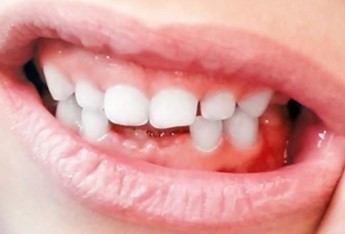
Case 3
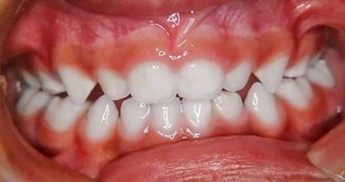
A mother brought her two-year-old and five-month-old son to the Schulzahnklinik in Basel after noticing changes in his dental positioning. The child presented with an anterior open bite and edge-to-edge bite on the first primary molars. The second primary molars were erupting. The patient no longer used a baby bottle but used the dummy almost constantly, both day and night. The dummy was replaced with a size two Curaprox soother. After three months of treatment, the bite was closed, and the second primary molars had erupted. A slight protrusion was observed, but the first primary molars appeared to be in a normal overbite. Weaning off the soother after treatment was not an issue.
Fig. 13
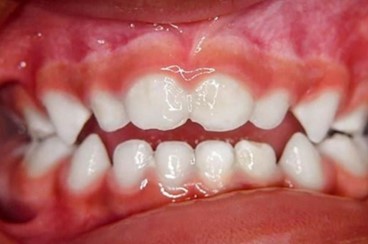
Fig. 14
Discussion
The Curaprox soother had a positive regulatory effect on the jaw misalignment in all three cases presented. Jaw misalignment was clearly linked to suckling habits. Unlike comfort soothers described in previous literature, the Curaprox soother features a unique pressure distribution that likely explains the corrections seen. When examining the model, pressure from below moves the side wings of the soother along the roof of the mouth, bypassing the palatine suture.
Conclusion
The initial results of using the new soother are encouraging. In order to develop an evidence-based recommendation, we need further tests covering the acceptance among children as well as the therapeutic and biomechanical effects. 
This article is a rewritten and summary of the original article; Filippi, C., Filippi, A., & Verna, C. (2015). Frühkindliche kieferorthopädische Therapie mittels Schnuller? Eine Fallserie. SWISS DENTAL JOURNAL SSO – Science and Clinical Topics, 125(9), 959-964.
References
- Miller J L, Sonies B C, Macedonia C: Emergence of oropharyngeal, laryngeal and swallowing activ- ity in the developing fetal upper aerodigestive tract: an ultrasound evaluation. Early Hum Dev 71: 61–87 (2003)
- Hack M, Estabrook M M, Robertson S S: Develop- ment of sucking rhythm in preterm infants. Early Hum Dev 11: 133–240 (1985)
- Fucile S, Gisel E G, Lau C: Oral stimulation acceler- ates the transition from tube to oral feeding in preterm infants. J Pediatr 141: 230–236 (2002)
- Barlow S M, Estep M: Central pattern generation and the motor infrastructure for suck, respira- tion and speech. J Com Dis 39: 366–380 (2006)
- Largo R: Babyjahre. Piper Verlag München: 462–463 (2001)
- 6. Hensel E, Splieth C: Gesundheitszustand, Mor- phologie und Funktion der 1. Dentition. Dtsch Zahnärztl Z 53: 398–402 (1998)
- Stahl F, Grabowski R, Gaebel M, Kundt G: Zusam- menhang von Okklusionsbefunden und orofa- zialem myofunktionellen Status im Milch- und frühen Wechselgebiss Teil II: Häufigkeit von orofazialen Dysfunktionen. In: Fortschritte der Kieferorthopädie Vol. 68: 74–90 (2007)
- Correa-Faria P, Ramos-Jorge M L, Martins-Ju- nior P A, Vieira-Andrade R G, Marques L S: Mal- occlusion in preschool children: prevalence and determinant factors. Eur Arch Paediatr Dent 15: 89– 96 (2014)
- Sousa R V, Ribeiro G L, Firmino R T, Martins C C, Granville-Garcia A F, Paiva S M: Prevalence and associated factors for the development of ante- rior open bite and posterior crossbite in the pri- mary dentition. Braz Dent J 25: 336–34 (2014)
- Voss E: Zahngesundheit, Gebissentwicklung und myofunktioneller Status bei Kindern eines Spracheilpädagogischen Förderzentrums. Med Diss Universität Rostock (2007)
- Dee D L, Li R, Lee L C, Grummer-Strawn L M: Associ- ations between breastfeeding practices and young children’s language and motor skill devel- opment. Pediatrics: 119 Suppl 1: S92–98 (2007)
- Nascimento Filho E, Mayer M P A, Pontes P, Pigna- tari A C C, Weckx L L M: Caries prevalence, levels of mutans Streptococci, and gingival and plaque indices in 3.0- to 5.0-year-old mouth breathing children. Caries Res 38: 572–575 (2004)
- Levrini L, Merlo P, Paracchini L: Different geomet- ric patterns of pacifiers compared on the basis of finite element analysis. Eur J Paediatr Dent Dec 8(4): 173–8 (2007)
- Salbach A, Grabowski R, Stahl de Castillon F: Der Einfluss orofazialer Dysfunktionen auf die Gebissentwicklung im Milch- und frühen Wechselgebiss. Quintessenz 63: 1427–1437 (2012)
- Zuralski H E: Klinische Studie zur Bewertung der kieferorthopädischen Bedeutung eines neuarti- gen Schnullers bei 27 Monate alten Kindern.
About the Author

Dr. Cornelia Filippi is a pediatric dentist and head of the prophylaxis department in the Clinic for General Pediatric and Adolescent Dentistry at the University Center for Dental Medicine Basel (UZB) as well as an active member of the Center for Saliva Diagnostics, Dry Mouth and Halitosis at the UZB.

Prof. Dr. Andreas Filippi is a specialist in Oral Surgery. He is the Clinical Director of the Department of Oral Surgery, University Center for Dental Medicine Basel UZB, Switzerland. Since 2006, he has been Founder and Head of the Center of Dental Traumatology Basel, and since 2016, Founder and Head of the Center of Salivary Diagnostics, Hyposalivation and Halitosis Basel.

Prof. Dr. Carlalberta Verna has been the Chair of the Department of Orthodontics and Pediatric Dentistry at the University Centre for Dental Medicine in Basel, Switzerland, since 2013. She earned her dental degree and doctoral thesis from the University of Ferrara, Italy, and completed two PhDs. Her research centers on bone turnover and orthodontic treatment analysis, with a clinical focus on treating patients with juvenile idiopathic arthritis and asymmetries.
link







