“Implementation Hypertension” in the pandemic era: unmasking white-coat effects in healthcare workers
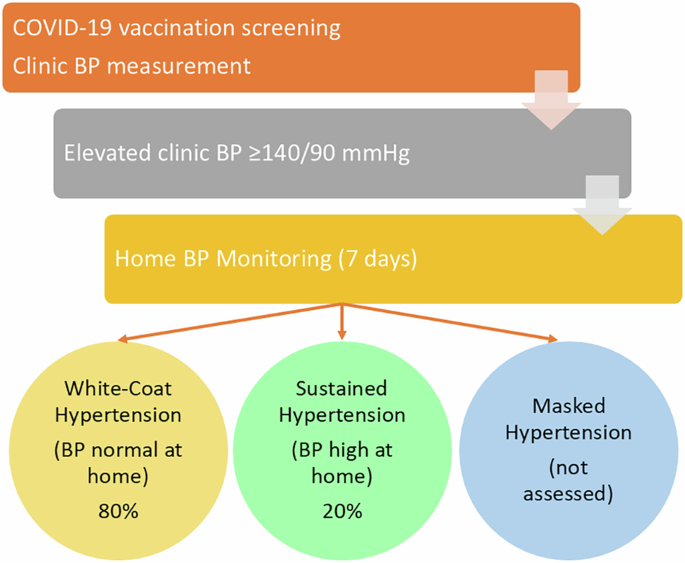
The COVID-19 pandemic created a large-scale opportunity for opportunistic blood pressure (BP) screening among healthcare workers. Mandatory pre-vaccination assessments required all healthcare workers to undergo clinic BP measurements, establishing conditions for observing a phenomenon recently termed “implementation hypertension (IH).” This refers to situations where hypertension is detected not in routine clinical settings, but through implementation-driven screening programs [1]. The study by Khamsai et al. reports that the overwhelming majority of individuals with elevated clinic BP during COVID-19 vaccination screening had white-coat hypertension (WCH), not sustained hypertension (SH) [2]. Specifically, 80% of those with high clinic BP were normotensive at home, highlighting the risk of misclassification if relying solely on clinic measurements (Fig. 1).
This study conducted guideline-based 7-day continuous home BP monitoring (HBPM) in 200 healthcare workers with clinic BP ≥ 140/90 mmHg. The finding that four out of five individuals with elevated clinic BP do not have true hypertension provides significant implications for hypertension research. Previous literature estimates the prevalence of WCH in the general hypertensive population to be 15–40% [3, 4]. The extraordinarily high proportion of WCH observed among healthcare workers during the pandemic period is thought to result from multiple overlapping factors. Healthcare workers experienced anxiety about vaccine side effects, increased occupational burdens, and psychological stress, all of which may enhance sympathetic nervous system activation and the white coat response [5]. Furthermore, when healthcare workers themselves become patients, their anxiety increases, and the white coat effect tends to be amplified compared to the general population [6].
This study further provides valuable insights into the predictors of SH and WCH. Increasing age, higher BMI, and a family history of hypertension were independently associated with SH, findings consistent with established cardiovascular risk profiles [7, 8]. Conversely, being female gender was strongly associated with WCH, consistent with prior studies indicating higher stress reactivity and differing emotional responses in women in clinical settings [9]. These distinctions hold practical significance, enabling clinicians to stratify patients identified through IH programs who are more likely to have true hypertension and prioritize follow-up evaluations.
As Khamsai et al.‘s findings emphasize, failing to confirm BP outside the clinic carries risks for IH programs, including overdiagnosis, unnecessary drug therapy, increased healthcare costs, and loss of patient trust. If diagnosis had been based solely on clinic BP, 80% of participants might have been incorrectly identified as hypertensive and started on unnecessary treatment. As large-scale community BP screening through digital health platforms and regional support is promoted globally, IH is suggested to become an essential component of worldwide hypertension control strategies. However, distinguishing transient BP elevation from true hypertension is crucial. Therefore, out-of-clinic BP measurement, particularly HBPM, must be positioned as an indispensable element in IH program design.
Another significant contribution of this study is the detailed analysis of morning and evening HBPM. The authors confirmed consistently elevated BP readings in both time periods among participants with SH, supporting the utility of HBPM not only as a diagnostic confirmation tool but also as a means to identify BP phenotypes. Morning hypertension and nocturnal hypertension are established indicators of increased cardiovascular risk. Integrating such phenotypic analysis into IH strategies may enable more personalized hypertension management (Fig. 1).
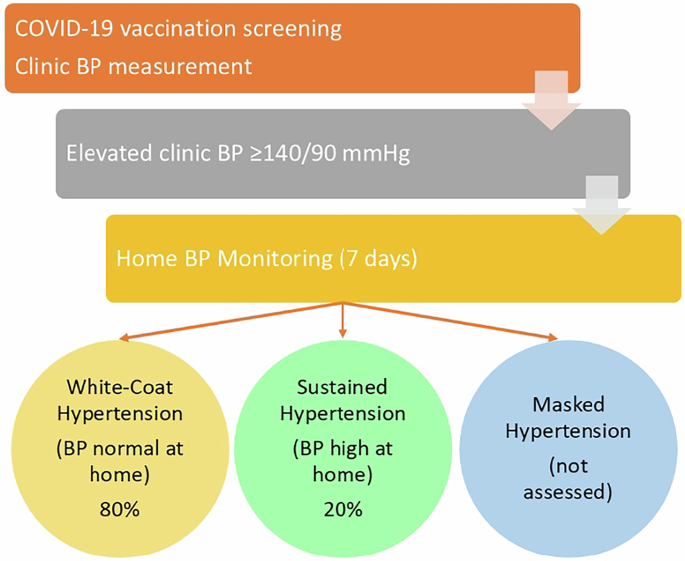
Conceptual graphical abstract illustrating the workflow and major findings of implemental hypertension (IH) detected during COVID-19 vaccination among medical personnel. Elevated clinic BP triggered home BP monitoring (HBPM), revealing that 80% of cases represented white-coat hypertension (WCH) rather than sustained hypertension (SH). The figure emphasizes the essential role of out-of-office BP monitoring in preventing overdiagnosis
Several limitations should be noted. This study was conducted at a single institution and included only healthcare professionals, limiting its generalizability to broader populations. Furthermore, while HBPM is widely recognized as reliable for identifying WCH, the absence of 24-h ambulatory blood pressure monitoring (ABPM) may have resulted in underdetection of masked hypertension. Future studies incorporating ABPM or wearable BP sensors may allow for a more comprehensive assessment of BP phenotypes in IH.
Khamsai et al. reported compelling risks associated with screening without confirmation. Their findings align with the international consensus that HBPM is a fundamental element of hypertension diagnosis. For the IH initiative to effectively contribute to global hypertension management, confirmatory digital BP monitoring must be incorporated from the outset, not as a secondary step.
In conclusion, this study demonstrated that opportunistic screening in high-stress settings, such as during pandemic vaccination, can inflate hypertension prevalence due to the WCH effect. Therefore, integrating HBPM or similar digital tools is essential for accurate diagnosis, preventing overtreatment, and ensuring guideline-based hypertension care. As hypertension management transitions into the digital era, the findings of this study contribute to patient-centered IH strategies.
link






