Suboptimal immunity of hepatitis B vaccination and seroprotection among healthcare professionals in a tertiary hospital in Ghana
The study evaluated the hepatitis B antibody response among a vaccinated group of Ghanaian healthcare professionals. Overall, 62% of participants achieved optimal seroprotection, with more than half showing antibody levels between 501 and 1000 mIU/ml. Nevertheless, a substantial proportion of vaccinated individuals did not reach the threshold for protective antibody levels, indicating variability in the immune response within this cohort.
Although vaccines are developed to offer protection, breakthrough infections have been documented, including among hepatitis B vaccinated individuals21,26,27. In the current study, we observed a breakthrough infection of less than 1%, and exclusively among participants with suboptimal antibody responses, suggesting that inadequate antibody levels can permit infection28. Our findings align with those of Obeng et al.21, which reported a 58% seroprotection rate and 2.4% breakthrough infection among vaccinated HCW in the Ashanti region. Similarly, a study among vaccinated HCW in the Cape Coast Metropolis documented a 91.8% seroprotection rate and a hepatitis B prevalence of 1%20. While our study observed a lower breakthrough infection rate, likely due to the smaller sample size, both studies highlight the persistence of suboptimal immunity despite full vaccination, reinforcing the need for post-vaccination antibody monitoring and identification of suboptimal responders among healthcare professionals in Ghana. Discrepancies in seroprotection rates may be explained by the timing of antibody testing, where antibody levels are known to peak 1–2 months after the final vaccine dose22,23, and testing outside this window, as was the case in our study, may underestimate the peak antibody responses. From a practical perspective, our findings highlight that a significant proportion of HCW remain at risk of HBV infection despite receiving the vaccine, primarily due to the absence of routine antibody titer monitoring in Ghana. Suboptimal immunity may arise from host-related factors, vaccine properties, handling, administration, or pathogen virulence29,30.
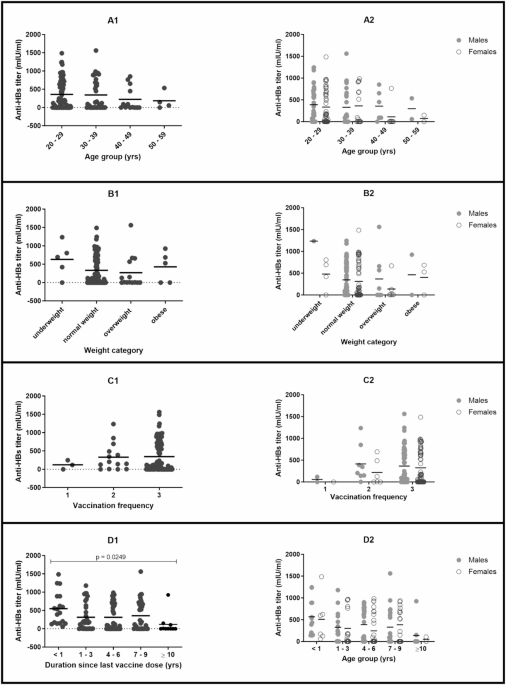
Demographic and clinical variables such as age, sex, BMI classification and vaccination frequency were not associated with antibody response when stratified into optimal and suboptimal groups. However, males, younger participants and those who received repeated vaccine doses tended to mount stronger responses. Consistent with earlier reports28,31, participants aged 40 years and above demonstrated lower antibody titers compared with younger individuals. Furthermore, antibody levels were elevated among those vaccinated within the past year than among those vaccinated earlier, suggesting waning immunity over time. This decline is consistent with the established immunological principle that antibody titers peak within weeks following antigen exposure and subsequently diminish gradually29,32.
Healthcare professionals are often exposed to the hazard of needle-stick injuries in the course of their duties, with an estimated 5.9% exposed annually to blood-borne HBV infections globally33,34. Robust immunity is therefore crucial to minimize vulnerability following accidental exposure. In our study, nearly 40% of HCW who may have initially demonstrated robust immune responses were at risk of reduced seroprotection between 1 and 3 years after vaccination. This underscores the potential value of adhering to post vaccination recommendations as set by WHO and CDC23,24 to identify HCWs who may not have developed the requisite amount of the antibodies needed to confer protection after the primary vaccination. Such individuals may benefit from revaccination.
Approximately 5–10% of healthy adults fail to mount adequate responses to hepatitis B vaccination35, highlighting the need to identify healthcare providers who remain unprotected. Current WHO and CDC guidelines23,24 recommend that all HCW should undergo post-vaccination serological testing for anti-HBs antibody titers 1–2 months after completing the vaccination to confirm adequate immune response (≥ 10 mIU/ml). This is critical for identifying individuals who fail to achieve protective antibody levels after two complete vaccination series (nonresponders) and for counseling them appropriately given their susceptibility. Although our study included all vaccinated HCW irrespective of the time since their last vaccination and did not specifically identify true nonresponders, it highlighted a 100% seroprotection rate among those vaccinated within one year. This finding contrasts with the report by Senoo-Dogbey and colleagues13, who observed a seroprotection rate of 91.3% among HCW from five selected hospitals in Accra, six months postvaccination. The discrepancy may be attributable to differences in study design or sample size, underscoring the need for larger, standardized evaluations to better characterize seroprotection rates among Ghanaian healthcare workers.
While hepatitis B vaccination confers substantial protection among HCW in Ghana, a considerable proportion fail to achieve optimal antibody titers over time. Seroprotection was highest among participants within one year of vaccination, suggesting waning immunity in subsequent years and underscoring the importance of timing in post-vaccination evaluation. Although true nonresponders were not explicitly identified, the presence of breakthrough infection among suboptimal responders emphasizes the vulnerability of this group. Taken together, these findings call for the integration of routine post-vaccination antibody testing into occupational health protocols in Ghana. Strengthening such measures is essential to safeguard HCW against occupational HBV exposure and to align national practices with international recommendations. It is recommended that management of healthcare centers should implement policies to screen and vaccinate all categories of HCW at the time of recruitment, followed by post vaccination measurement of antibody titers, which will be cost effective compared to post-exposure prophylaxis with immunoglobulins.
Study limitations
Whilst the study has important findings, there are notable limitations. First, the cross-sectional design limits the ability to infer the dynamics of antibody persistence over time. Secondly, post-vaccination serological testing was not conducted within the recommended 1–2 months following vaccine completion when antibody titers peak, this may have affected the identification of true nonresponders. Additionally, the study did not include testing for anti-HBc, which would have distinguished immunity from natural infection from vaccine-induced protection. Finally, the sample size, while adequate for descriptive analysis, may have limited the statistical power to detect smaller associations with demographic or clinical factors.
link






